
Note: All images and content in this blog post are copyrighted and belong to Elizabeth Abrahamsen. This blog post may not be reproduced in part or in whole on any other website or page. Any reposting of images or text from this page is subject to legal action.
One day in November 2020 Eric and I noticed Trevor doing this ridiculously adorable Woody the Woodpecker kind of giggle laugh. We just thought it was a new thing he picked up and we laughed too every time he did it. The weather had abruptly changed that week as it often does in central Texas in November and a cold snap had brought the temperatures plummeting 20 degrees overnight. In the afternoon he was coughing a little bit and I started hearing a wheezing in his chest that troubled me, so I let him sleep in the bed with us that night. He slept very fitfully, and my concern grew. When my best friend, Michelle, was on hospice from colon cancer in March 2019 her sister in law, Sarah, who had spent years as a hospice nurse before moving into trauma, had talked to everyone who was watching out for Michelle. “When people can’t breathe, they get agitated or restless, they might get really irritable and cranky, and get up and walk around,” she told us. So around 5 AM I woke up to Trevor whimpering, fidgeting, and kicking his feet. The wheezing had become alarmingly loud. I got him up and took him to the guest bathroom because it’s small and I can build up a really good steam in there. I knew that steam could help kids breathe when they have croup, so I decided to try it. After a while in the steam though, he was still wheezing and cranky. Eric got up and was talking to us. I was thinking we might need to bring Trevor to the ER, but there was still one other thing to try first. I had been prescribed an inhaler by a doctor a while back that I had never used. I grabbed it, read the instructions and brought it to Trevor. He was only four at the time and speech delayed, so I didn’t expect him to be able to take it properly, and I was marginally afraid it might make it worse, so I squirted it in front of his open mouth and told him to breathe. He did, and I could tell an immediate difference in the wheezing. His labored breathing eased a bit and his body visibly relaxed.

I have no experience with asthma. No one in my family has it. I’m pretty sure the doctor who prescribed me the inhaler did so in response to what was almost certainly a panic attack in actuality. Anxiety and I are old nemeses. Trevor stabilized well enough that evening that I no longer felt like he needed to go to the ER, but I did stay up and make him a doctor appointment for the earliest time slot I could get. When I brought him in the next day, the nurses attached a pulse oximeter to his finger and they looked confused. “What’s wrong? Is it not giving you a reading?” I asked. She laughed a little uncomfortably and said, “Well it’s telling me his blood oxygen is at 87 but I don’t think that’s accurate because he should be gasping.” He wasn’t gasping. He was sitting quietly. The doctor came in and examined him and prescribed him his own albuterol inhaler with a special attachment that helps children learn to use an inhaler. She said “We can’t diagnose him with asthma until it becomes a pattern, use the inhaler if he is wheezing again, and I’m prescribing an oral steroid that you can use first if you think he might need to go to the ER.”
So we used the inhaler for the next few days. We also tried the oral steroid, but it made him vomit violently and immediately. I went ahead and ordered a pulse oximeter off Amazon so I could check his oxygen level myself periodically. It remained high in the coming weeks, 97 and higher every time, so I put it in my purse and we went on about life. Anytime the woodpecker laugh or slightest wheeze returned I checked his oxygen levels and sometimes gave him his inhaler.
Several months ago I brought him in for a strep test with a different doctor at the same clinic. He picked up a wheeze in the stethoscope that I couldn’t hear with my normal human mom ears. “Go ahead and use the inhaler every four hours for the next few days, and you can use it anytime he has an upper respiratory illness going on.” So I went off with those instructions in hand and began using the inhaler more frequently. He stopped seeming to need it though so we put it away for a while.
On Wednesday this week Trevor started having a very mild, dry cough. It didn’t affect his energy levels and he didn’t have any fever so I let him go on about his normal business, going to school and playing t-ball. On Wednesday night he had a really bad night terror episode where he was running from room to room and screaming, seemingly awake but inconsolable. This happens from time to time, especially when he gets over tired, but it’s never been this bad before. He went back to sleep and slept late Thursday morning.

He had a t-ball game Thursday night and played hard, I knew he would be exhausted, so I got him dinner and a bath and gave him some Mucinex and inhaler to head off the coughing, and put him to bed next to his humidifier. He coughed really hard all night, and woke up at 2 AM needing more cough medicine and inhaler. He had a hard time going back to sleep and kept asking, “Is it morning yet?” When it was morning we gave him some more inhaler and he went immediately back to sleep. I was supposed to go to a MOPS leadership meeting that morning, and I briefly considered leaving him to convalesce on the couch while his Dad worked from home, but the coughing had worried me, so I let the rest of the team know I wouldn’t be there. While Trevor snoozed in my bed I got the girls off to school and then made him an appointment to see his pediatrician at 1:45. I came in to check on him around 8 and noticed him wheezing a little bit and he was doing what I call “tummy breathing” where his stomach is visibly coming up and down. It is an obviously labored breathing move to make while unconscious asleep. It was also sort of a weird pattern, very rapid intake of breath with an exhale about 3 times as long as the inhale. “Ah-WHOOOOO, ah-WHOOOOO, ah-WHOOOO”
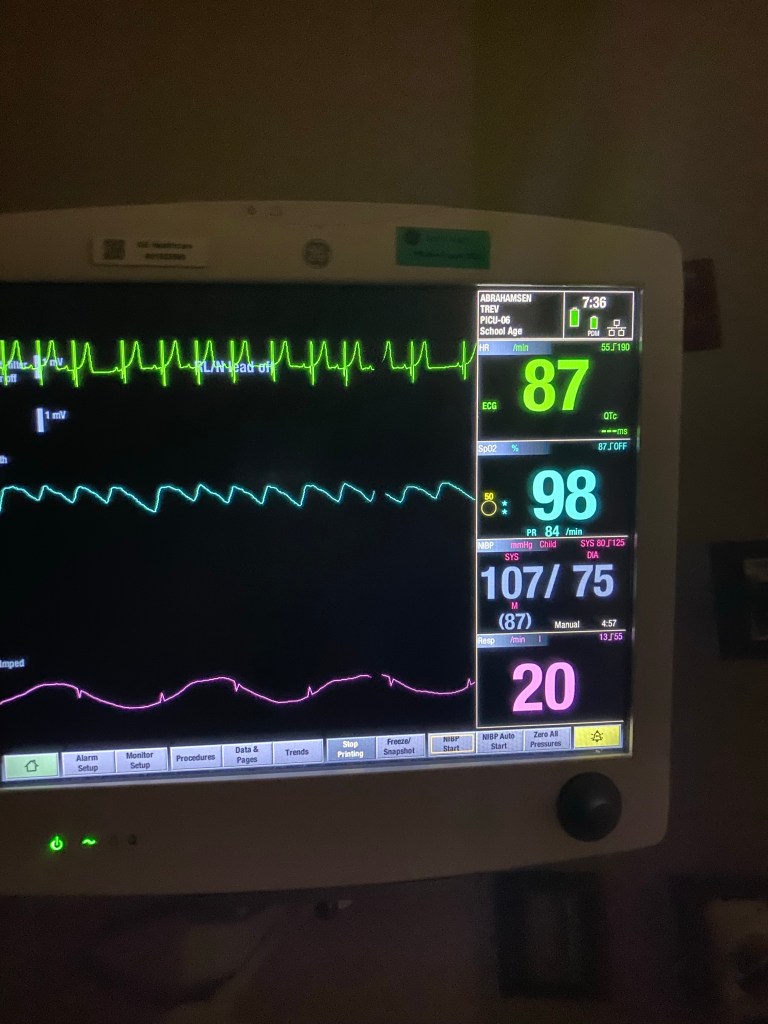
This started asthma alarm bells ringing in my brain, so I got my pulse oximeter and woke Trevor up. The first reading was 87/161. I took a reading on his other hand and it resulted in similar numbers. I gave him one more puff from his inhaler but I hesitated to give him more because I didn’t know if he could overdose on albuterol. His o2 stats went up to 90 right after the puff, but immediately back down into the 80’s.
I texted my neighbor (who is a nurse) the numbers and asked her if I needed to bring him to the ER, and she said, “Well his oxygen is low and his heart rate is high so he should see a doctor.” I told her about the afternoon appointment and she advised me to try to get an earlier one. “Anything below 90 is unsafe,” she said.
I was able to get Trevor an appointment at the clinic at 9:50. In the meantime I tried to give him some prednisolone. I had figured out that he could sometimes handle it if I gave him 1 milliliter at a time with food and water and at least three minutes between doses. I had never been able to give him more than 6 ML total even though the dose is 12 ML. I thought, It’s worth a try today though, so we tried it. He couldn’t handle one milliliter. He didn’t even make it to the bathroom, he threw up all over the floor in the living room. He was really upset, so I put him in the bathroom in a bubble bath and went to clean up the vomit mess. I got him some clean clothes and moved him forward in the tub, pointed the shower head at the opposite wall and turned up the temp and closed the bath curtain to create a steam bath. I got myself dressed and ate something and we headed in to the clinic about 20 minutes early.
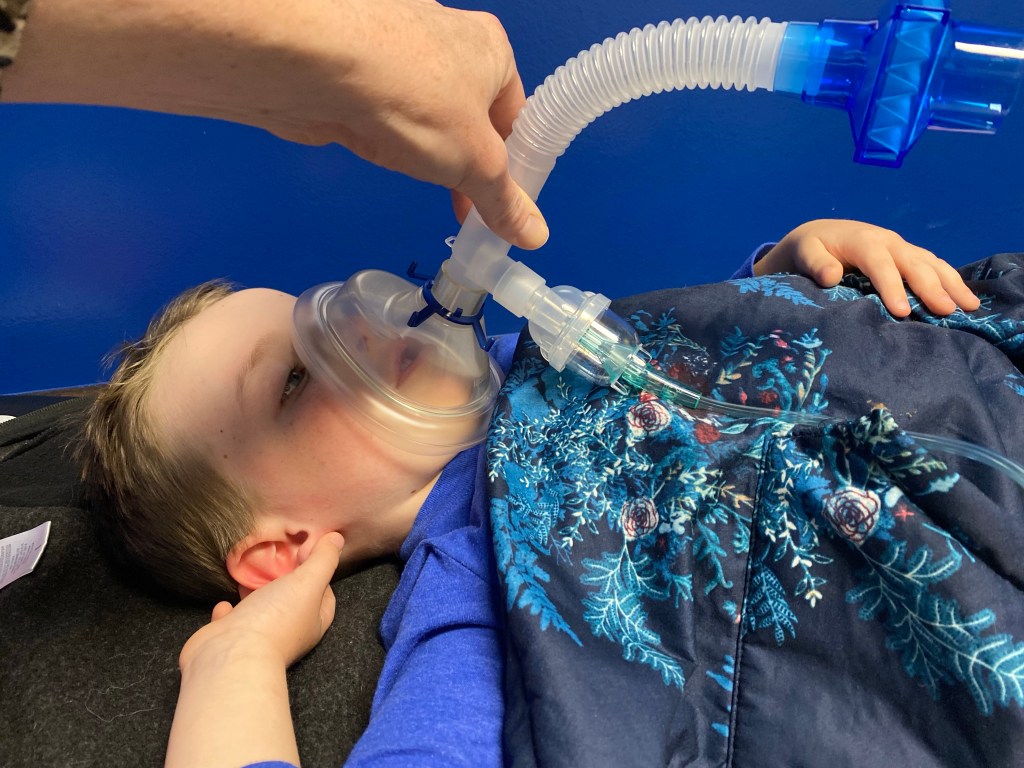
Thankfully they were able to see us right away, and they acknowledged his numbers were concerning. They had me give him more albuterol and waited, then took a reading. The numbers were still low, so we repeated the albuterol/wait method with the same non-effect. The next step was to try a different oral steroid which the doctor said some kids can tolerate better, and thankfully he did keep it down, but again his numbers didn’t stabilize. After that they wheeled in an oxygen tank and gave him 10 minutes of oxygen. His oxygen saturation went up to 96, but it dropped back into the 80s after he was taken off. They tried that one more time with the same result, and at that point they said, “He may need hours of oxygen, it is probably the best idea to go to a pediatric ER.” So they sent me with the appointment notes and I drove over to the children’s ER at St. David’s and had Eric meet me there.

They got Trevor back right away and sent in a respiratory therapist who got him on oxygen and gave him an hour long albuterol nebulizing breathing treatment. At that point it was after 2 PM, none of us had had any lunch, and Vivienne was going to be home at 3, so Eric sent me home to shower, eat and be there for Vivienne while the hospital embarked on a second hour long breathing treatment for Trevor.
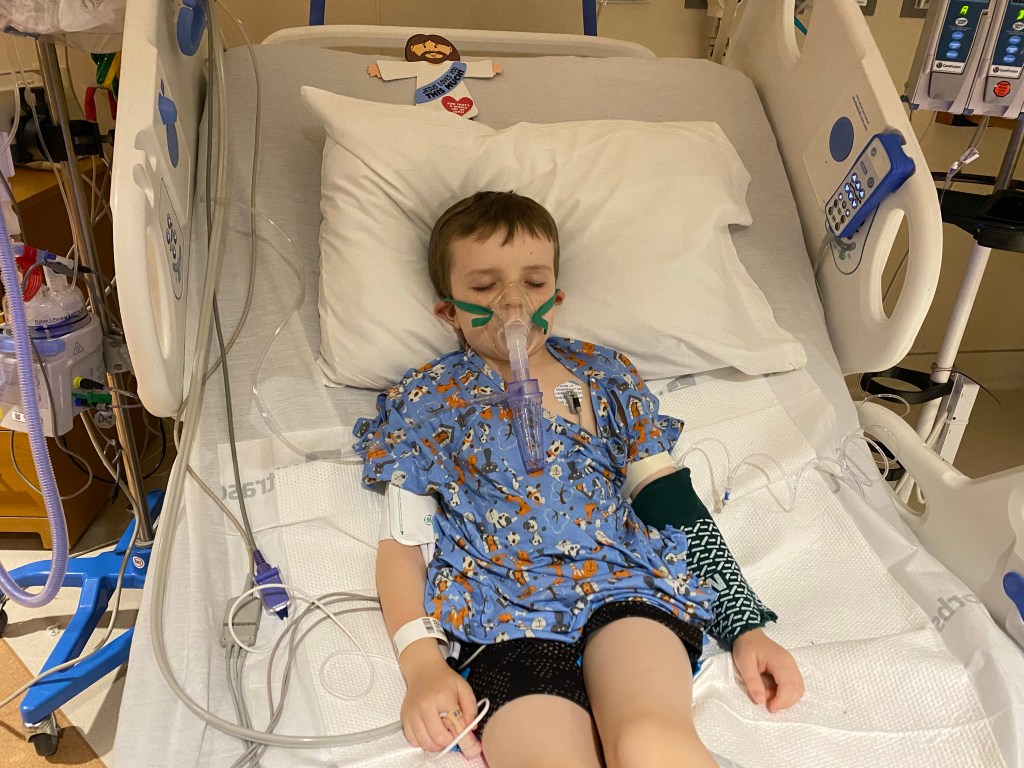
At home Eric called and let me know they were going to prep Trevor for an IV, and he would likely be admitted until at least Sunday. I waited for Bella to get off the bus and packed a small bag for Eric and myself and Trevor and headed out to the hospital with the girls.
They admitted Trevor to the PICU and he received constant oxygen and albuterol for the first 24 hours. He was initially very sleepy which is understandable with his heart rate ranging from the 140s to the 160s all day long with his blood oxygen level being in the 80’s. The pediatrician at the clinic Friday morning said, “As far as his body knows, Trevor is climbing a mountain right now, he is physically exerting himself, and the air is very thin.” In the PICU they had to switch from a face mask to a nasal cannula and wow he really did NOT like that. Eric and I had to hold him down and I got kicked in the face. His little eyes were all glazed over and he didn’t seem like himself, so it was pretty terrifying. Eventually he calmed down after they gave him some IV Precedex. Eric really wanted to stay with him and the PICU doesn’t allow visitors under the age of 18 so I took the girls home for the night. That was probably a good plan because Eric has a cool head in a crisis, and I definitely don’t. So I came home and called everyone to let them know what was going on, and tried to comfort my girls who were both handling their brother’s sudden hospitalization in different ways. Vivienne had a ton of nervous energy and was crying and needed lots of hugs and reassurances. Bella’s fear was manifesting as irritation and anger, which was mainly directed at Vivienne. She needed a lot of alone time to process. I personally needed to clean. I was home less than 24 hours but I cleaned my bathroom and kitchen and laundry room and vacuumed the downstairs.
The next day we headed back in to the hospital, and I switched off with Eric. Teresa (Eric’s mom) came to see Trevor at the hospital and he got Balloons and toys from all of us. His energy was much higher that day but his numbers only stayed in an acceptable range while he was medicated.

Sometimes the alarms on the monitors would be going off and Trevor was still happily playing, seeming perfectly healthy.
One of the hospital employees from Child Life, Maggie, brought Trevor a mat to play on as well as play-doh and matchbox cars. She put an IV on Trevor’s stuffie, a red panda named Combo Panda. Trevor was immediately attached to Maggie. He started calling her “The Teacher” and kept asking “When is the teacher going to come back?”
Bella and Vivienne and I brought Trevor some balloons and toys including a spider man ball that Bella chose for him.
The hospital staff did a nasal swab and ran a respiratory panel which resulted in positive for rhino virus and enterovirus, which are both just colds, but nonetheless, that is what was responsible for putting Trevor in the PICU, with possible contribution from high pollen counts.
On Saturday they amended the original estimate of discharge from Sunday to probably Tuesday. Teresa went home to stay with the girls so Eric and I could both stay at the hospital. My family was fed by my sweet friend Lourdes who brought over homemade arroz con pollo and muffins! Our neighbor mowed our front lawn for us, and we felt very loved.
On Sunday they began weaning Trevor from the oxygen and albuterol, and Eric stayed at the hospital that night so I could get the girls off to school Monday morning. My friend Stacy brought our family dinner from Moonshine, and my friend Lisa brought us homemade strawberry muffins made with fresh strawberries for the girls to have for breakfast.

On Monday I brought Eric some breakfast and switched off with him so he could go home and get some work done. Teresa brought Trevor some Wendy’s chicken nuggets, which he had been asking for, and a huge bag of sour patch kids! Also Maggie came to visit, so Trevor was very happy. We figured out that we could roll/bounce the spider man ball to each other and that was very fun for my bored little guy.
On Monday morning they switched Trevor from IV meds to oral meds, and on Monday evening they removed his nasal cannula. My friend Jenna brought Trevor a big bag of toys and treats from the MOPS Leadership team and he had a blast opening and playing with all the treats!

On Monday night Trevor threw up his oral dose of prednisolone, but thankfully they didn’t make him take it again. He slept well and didn’t desaturate in the night, so on Tuesday morning they started our discharge process and by 11:30 we were on our way home!
Trevor hadn’t seen his sisters since Thursday because he wasn’t awake when they left for school on Friday morning, and he was already in the PICU by the time they got out of school on Friday. Unfortunately, minors aren’t allowed as visitors in the PICU so they had to sit in the waiting room and use FaceTime to talk to their brother. So when they finally saw each other again they hugged for a really long time and it definitely made me cry.


Afterwards we went to go get Vivienne’s sweater which she had left at the playground, and Trevor wanted to play. He had been cooped up for so long but I also didn’t want to strain him so I set a 10 minute timer and let them play. It turned into a mini Yes Day because after that they had popsicles at home, and then asked if they could have a water balloon fight. Yes. All the things. Our baby is home! Everyone had fun and didn’t get mad at each other which is a common issue with water balloon fights. Then they all had a bath because they were soaking wet and covered in grass.


My mom came into town on Wednesday to see Trevor and to help where she could, and she stayed to celebrate Easter with us!

On Wednesday Trevor’s teacher came to visit and brought us get-well-soon cards made by his whole class! In the afternoon we met with the Pulminologist who got us an asthma action plan and answered all 1,000 of my questions. Friday we followed up with Trevor’s pediatrician, who referred us to an allergist. He was still coughing on Sunday, so we decided to stay home and do online church for Easter service. Even though rhino virus and enterovirus are just colds, we didn’t want to run the risk of putting anyone else’s asthmatic child into the PICU.
It will be an adjustment – it already has been – learning to live with asthma. When we came home we were giving Trevor breathing treatments every four hours, even throughout the night. I thought, Well, it’s not much different from waking up all night long to nurse him as a baby. In the hospital I asked the doctor if Trevor could still play T-ball. “Absolutely,” he responded. “Jackie Joyner Kersee has asthma. Michael Phelps has asthma. Trevor can still play t-ball. You just learn to spot his triggers and keep up with his treatments. With asthma, you have two types of meds: rescue and control. The albuterol and prednisolone are rescue; they work fast too give temporary relief. The flo-vent is control; you give it daily to prevent attacks.”
Another one of the hospital doctors prepared us for the possibility that we may end up in the hospital once a year or so for a while. I hope she is wrong, but I would rather have a doctor who levels with me than lies to me. For now we are keeping a watchful eye on our little guy and praying he can go back to school and somewhat normalcy by Tuesday.

We are still learning how to live with asthma, and what role asthma will play in the story God is writing for Trevor’s life, but I look at this whole situation as God’s mercy. Trevor got the help he needed, and incredible care. If he had had this big episode first, instead of the smaller one in November, I don’t think I would have known it was asthma. If I had left him home all day to convalesce on the couch I have no idea what damage would have been done. I know that God’s works aren’t always done through miraculous healing, but instead many are showing His power in the lives of people who are afflicted. Whatever His plans for Trevor, I know that He is good, and He can be trusted, and He loves my son much better and bigger and more completely than I ever could.
All images and content in this blog post are copyrighted and belong to Elizabeth Abrahamsen. This blog post may not be reproduced in part or in whole on any other website or page. Any reposting of images or text from this page is subject to legal action.

One thought on “Learning to Live With Asthma”